A tweet by NHS consultant oncologist Clive Peedell led me to some data on the funding for GP services in the NHS and the demand that there is for them.
The data is to be found in a Royal College of GPs press release from 2014 referring to a report they had commissioned from Deloitte.
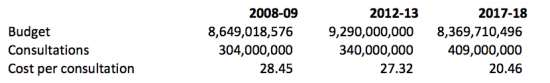
Using this data and the assumptions I note below the funding per GP consultation in England has, or will, change as follows over a period of a little less than a decade:
Let me be clear how I worked this.
The prices are constant 2014-15 data and so are directly comparable.
I assumed the real terms budget for the NHS in 2017-18 would be the same as that in 2015-16, which is fair.
The data on number of GP consultations comes from the RCGP.
The RCGP data is for England: I assumed the English budget for GP services is a constant ratio to the total GP budget over the period. This may not be precisely accurate, but is unlikely to make any significant difference at all.
I assumed the GP proportion of the NHS budget was the same in 2008/09 as it was in 2012/13 as I could not see alternative data for that.
What is clear is that, first of all, there is a massive increase in demand for NHS GP services. The data is real from 2008/09 to 2012/13: there is no reason to doubt the trend given the decline in other services available to the public.
Second, as the RCGP have pointed out, there is a real decline in the proportion of a relatively modestly increasing overall NHS budget now being allocated to GP services.
And the outcome is that GPs are now, in real terms, going to be given just 72% of the funding they had in 2009/09 for each visit in the future, or have to be 38% more efficient.
Since time with a patient, or working more hours, is just about the only variable available to a GP, it's not hard to see how the quality of GP services is declining, patients are losing out and that there are more and more GPs quitting, leading to a crisis in GP services as more and more practices have to close their lists to create safe working conditions.
To put it another way, austerity simply does not work, especially if you care.
Thanks for reading this post.
You can share this post on social media of your choice by clicking these icons:
You can subscribe to this blog's daily email here.
And if you would like to support this blog you can, here:



Just caught the tail end of a piece on Today this morning. That Stephen Dorrell, Alan Milburn and another MP are to look at funding the NHS. As both have links with private healthcare, it is surely, as usual, putting the fox in charge of the hencoop.
And as usual, telling us how the aged are putting such a strain on the service. I guess I shall be out on the ice flow soon when all my teeth have gone.
Agreed: this is just an exercise in privatisation
Lib Dem Norman Lamb was the third, i think
My questions are:
1. What constituted this rising demand, i.e. referrals, presentations, assessments, etc.?
2. How much of it is “failure” demand. To illustrate this second point, here is an excerpt from an article by ex-Observer business columnist, Simon Caulkin (blog: Sun, 24th Mar 2013):
“A chart produced by Vanguard Consulting of hospital accident and emergency (A&E) admissions shows that in three NHS hospitals studied five per cent of patients consume almost half the resource. (Good example of the Pareto principle)
The urgent question is: who are these needy patients? Sufferers from chronic cancer or other serious conditions? Accident or violence victims needing extensive reconstruction? Diabetes or obesity sufferers? Nope. Four out of five of them are people with chaotic lives — homeless, drug or alcohol users, or any combination of the above — who shouldn’t be in A&E at all but constantly re-present for minor ailments because their problem hasn’t been solved elsewhere. The buck stops at the NHS — which picks it up, assesses it and spits it out again and again, learning nothing in the process.
In other words, 40 per cent of the entire A&E resource goes up in failure demand — demand created by a failure to do something or do something properly the first time round; demand that shouldn’t be there — in many cases because of limitations in social care.
What we have here therefore is not a health economics, but a management, problem.”
As I have said so often before, we do not investigate demand sufficiently in the economics discipline.
Demand has risen since john Major encouraged people to think of themselves as health service consumers
Richard, that is a guess – unless you have evidence. My supermarket tells me I want cheaper goods. That does not make me buy any more or even look for them.
As I said, we really, really need to understand the nature of NHS demand, if we consider ourselves any kinds of economists.
There are many people working on that
I do not claim to be an expert